Personalized recommendations based on your needs
A Message From Our Medical Director
Psychiatric Care & TMS Therapy for the Greater Puget Sound of Washington
Real Care,
From a Team That Gets It
We know how frustrating it can be when you’ve tried things and still don’t feel better. That’s why we offer care that adapts to you - from traditional options like therapy and medication to modern tools like TMS and genetic testing.
Everything we do is built to support your healing, your way.

Personal
Care Team
Compassionate and Experienced
We combine science-backed treatments with compassionate care to ensure that each patient receives the support they need. Our team of highly trained mental health professionals works closely with individuals to develop personalized treatment plans that align with their goals, lifestyle, and unique needs.
Treatments We Offer
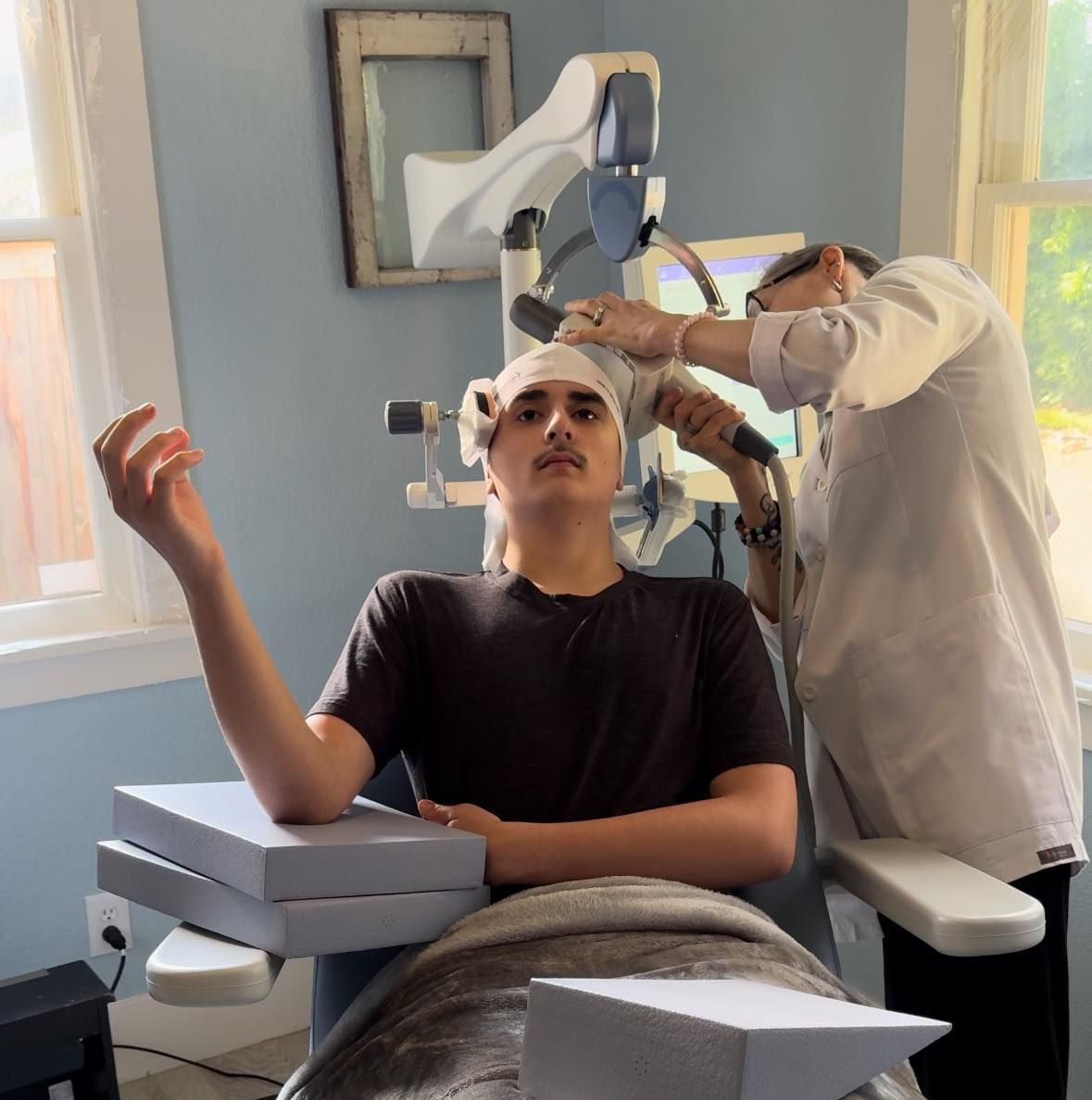
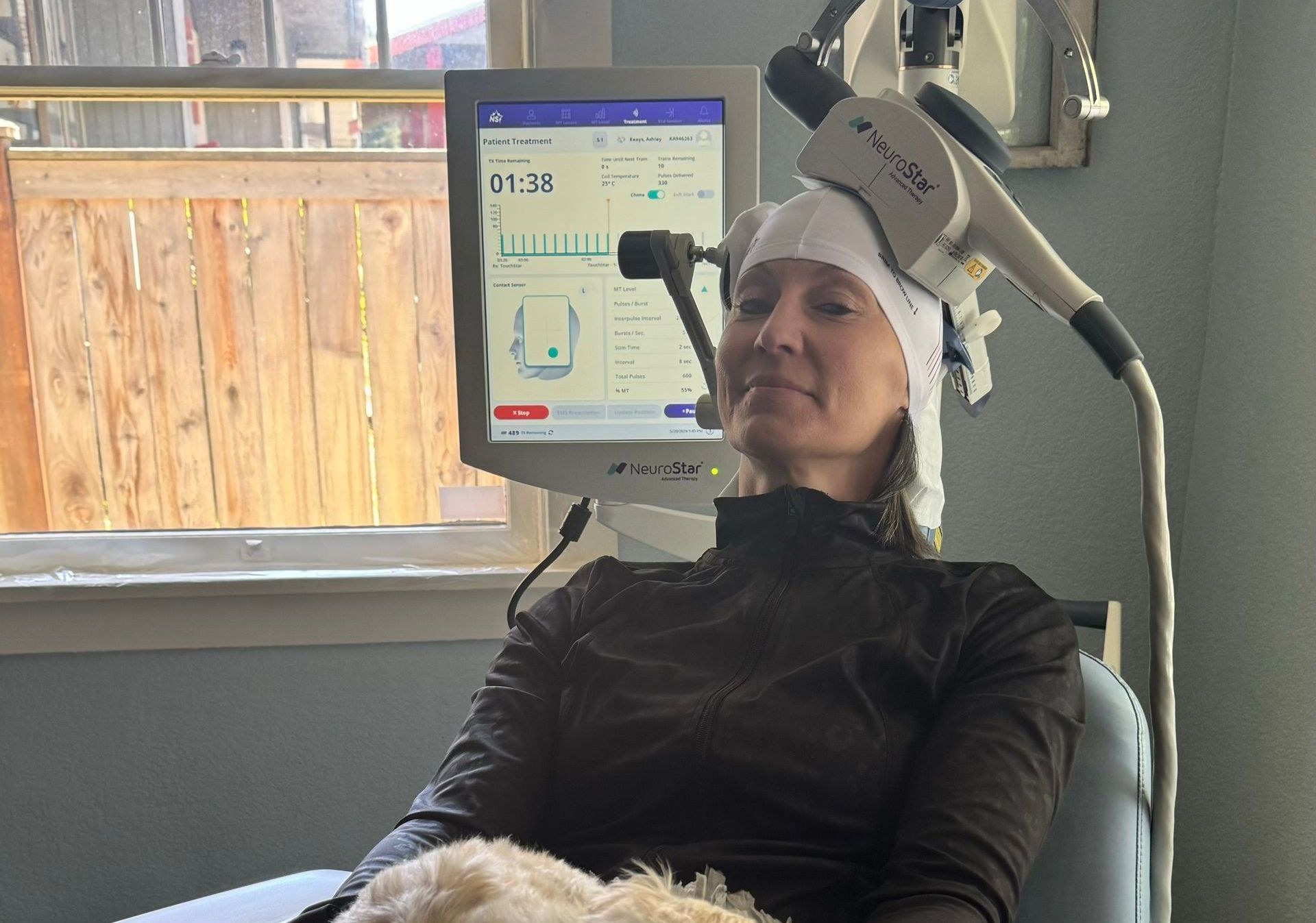
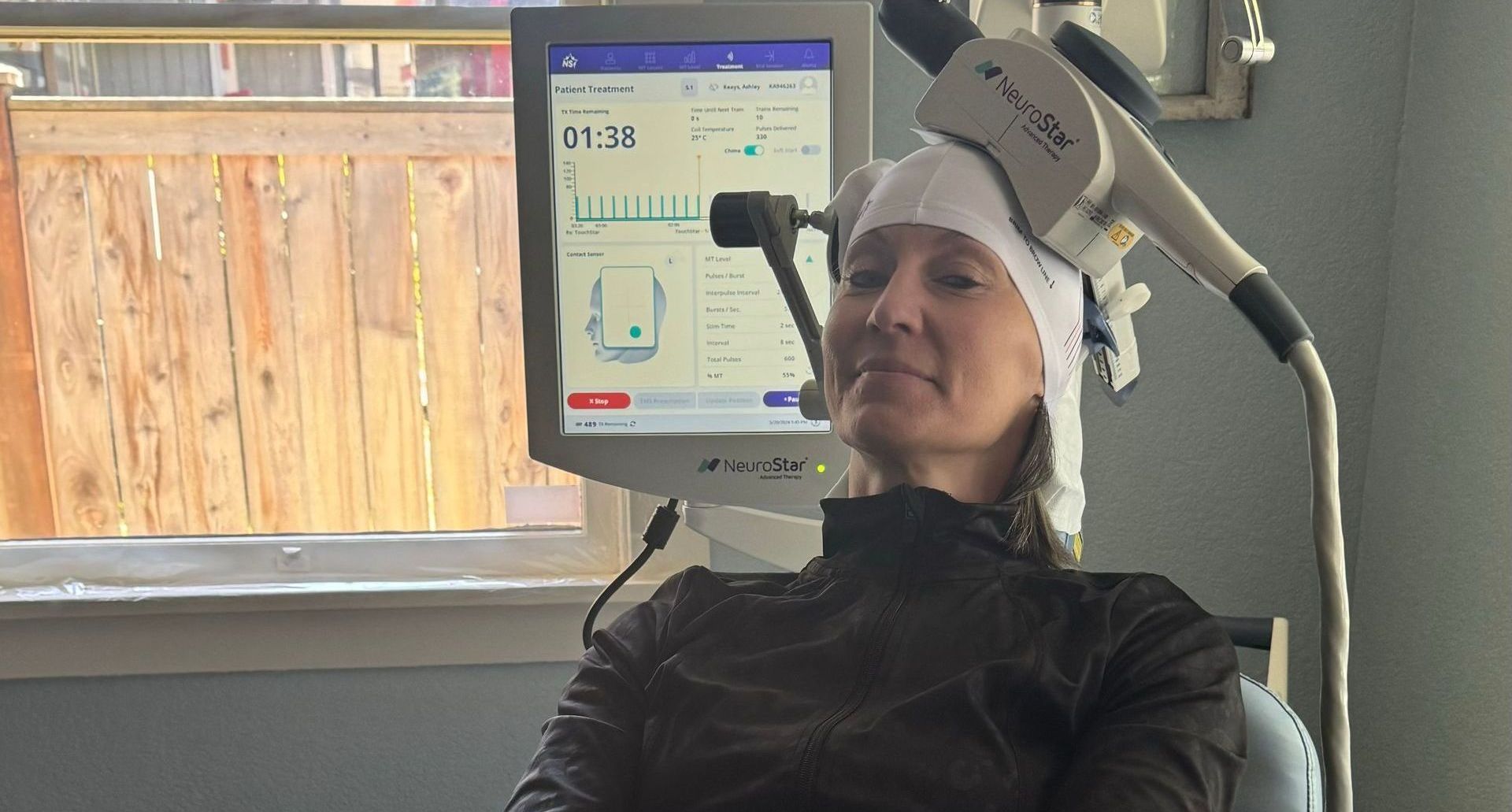
Creative Wellness TMS offers a full spectrum of mental health services, including talk therapy, medication management, and advanced interventional psychiatric treatments like Transcranial Magnetic Stimulation. Each service is thoughtfully designed to support your unique needs.

83%
of patients experienced symptom improvement, with
62% achieving full remission
after completing TMS.
"From the first visit, Creative Wellness exceeded my expectations. Dr. Keays and her staff are genuine, the results are real, and the atmosphere is empowering. The care that I received from Creative Wellness has transformed my life enormously."
"I cannot say enough about Creative Solutions, Dr. Simonsen, his staff, and TMS. I was skeptical but decided to give it a try. They were very thorough in explaining the what's/why's/how's and extremely professional every step of the way. I feel better than I have in YEARS."
"TMS therapy was super helpful, I came to him with severe depression and taking meds that helped very minimally! I was impressed with how quickly I noticed changes with my mental health and my desire to actually want to get up and do things where as before I had zero desire for anything! "
Tailored Care, Built Around You
Featured Resources





Request Appointment
For more details or to schedule a consultation, give us a call at 253-900-1605 or fill out our online form.